
Dr. Nancy Redfern is a consultant Anaesthetist in the UK, with clinical interests in obstetric and neuroanaesthesia. She was appointed in 1987 and, as a training programme director for many years, she became aware of the many barriers to the development of young doctors. She was also Vice President of the national Association of Anaesthetists, where she did much of her work related to safety standards and to the wellbeing of clinicians. She is involved in the Fight Fatigue campaign in the UK, and in its European counterpart, the Fighting Fatigue Together campaign coordinated by EUPSF.
Why does the wellbeing and safety of the healthcare workers personally matter to you?
The more I worked with trainees and in different multi-professional clinical teams, the more I realised that we deliver better care to patients when our workload is realistic, and people feel respected and valued as individuals. If the staff are looked after, they deliver safer and kinder service to patients.
In recent years, as the complexity of patient care has increased, and patients have rightly expected higher standards of care, more interest has been paid to the importance of the wellbeing of healthcare staff. We all want to be cared for by people who enjoy their jobs, who work in good teams and who have the resources to deliver the best care.

At a certain point in your career, you decided to take up the fight against healthcare professional fatigue. Why?
Over time, I began to see more and more signs that the level of fatigue among the medical staff was increasing in a worrying way. And in 2017, the untimely death of a trainee in a car accident driving home tired after a night shift convinced me we needed to take action to address staff fatigue.
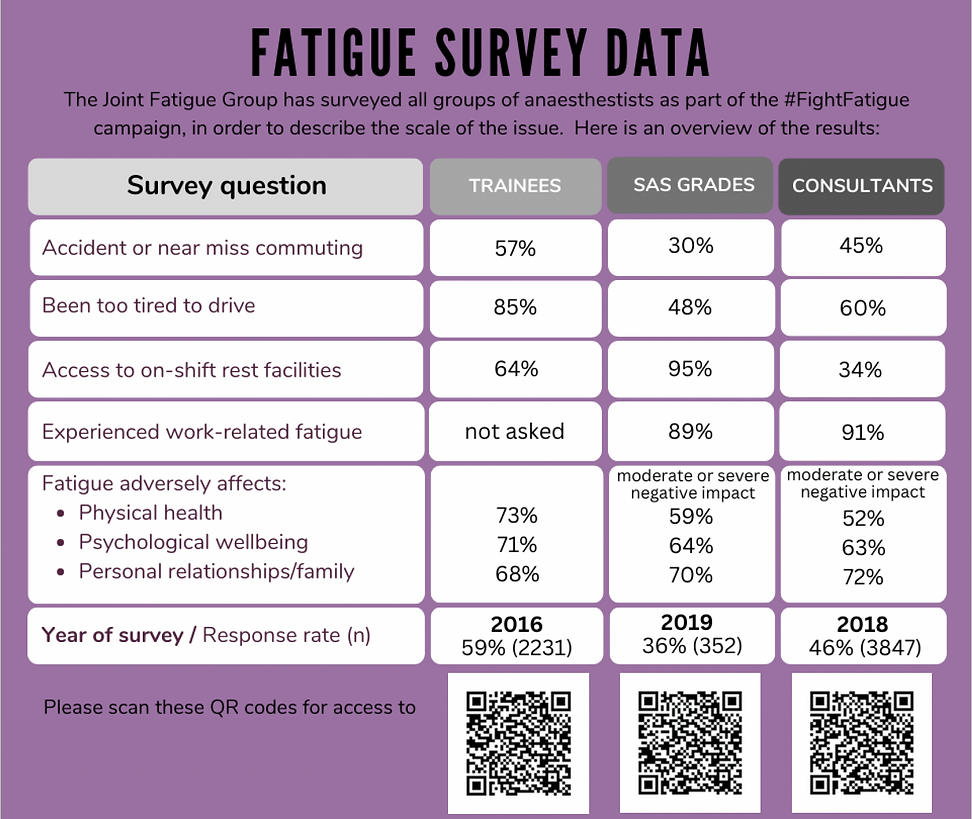
Together with a group of trainees and consultants and with the support of the Association of Anaesthetists, Royal College of Anaesthetists and Faculty of Intensive Care Medicine in the UK, we established a joint working group on fatigue. We organised a survey and found that 57% of trainees and 45% of consultants had had an accident or a near miss driving home tired, and many had no rest facilities at work. We clearly had a problem.
As a medical professional, how would you describe your experience with fatigue?
When I was a trainee, fatigue was regarded as an occupational hazard; we were expected to cope and working long hours was regarded as a badge of honour. We had almost no understanding of why we need to sleep and the impacts of sleep deprivation on us and on our clinical performance. However, we did have on call rooms and rest facilities.
Over the last 30 years, working hours have been cut by half as doctors expected a better work-life balance. But work has become more complex, more stressful and patients rightly expect more involvement in their treatment. Many trainee doctors work 12-hour night shifts and no longer have an on call room to sleep in.
From a professional point of view, this is obviously problematic, as fatigue affects how we think and behave in ways we may not notice; how we assess risk, make decisions, perform complex tasks, interact with colleagues, and manage our emotions. Attention, memory, response times, vigilance, hand-eye coordination, arithmetic ability and impulsivity are all affected.
In a few words, what will you be focusing on at the conference?
I would like to explain what we’ve been able to do in the UK to try and change the approach to fatigue – both culturally and practically – in hospitals and at a political level, with the aim of making it easier for people who are interested in the problem to take action elsewhere in Europe.
Because I believe that the fatigue of healthcare professionals knows no borders. In many European countries, there are shortages of many healthcare professionals: nurses, doctors, radiographers, pharmacists, etc. Patient demand is increasing with an older, less healthy population, so healthcare professionals do their best to keep the service going, working harder to cover gaps. Naturally this takes its toll and people end up getting used to chronically shorter sleep and don’t recognise its impact on their wellbeing. Where people work in challenging and unsupportive environments, this can even lead to burnout. Much needs to be done, and I think that a European network such as the Fighting Fatigue Together, which I have joined, can help to tackle this issue more effectively across Europe.

Finally, I’d like to open the discussion to what I consider to be an essential topic: the management of fatigue as a risk in the medical sector. All other safety-critical sectors are required by law to manage staff fatigue effectively as part of their overall safety structures. Healthcare workers have the same physiology as airline pilots and nuclear workers, so the medical sector should have the same regulatory framework. Good fatigue risk management could improve staff and patient safety, staff morale and staff retention.
Dr Nancy Redfern
EUPSF Advisory Board Member
Co-chair of the Joint Fatigue Group (UK)
WELL-BEING AND SAFETY OF THE HEALTHCARE WORKERS
Fighting Fatigue Together – Collaborating across Europe
